
- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Search
- Page Path
- HOME > Search
- Complications
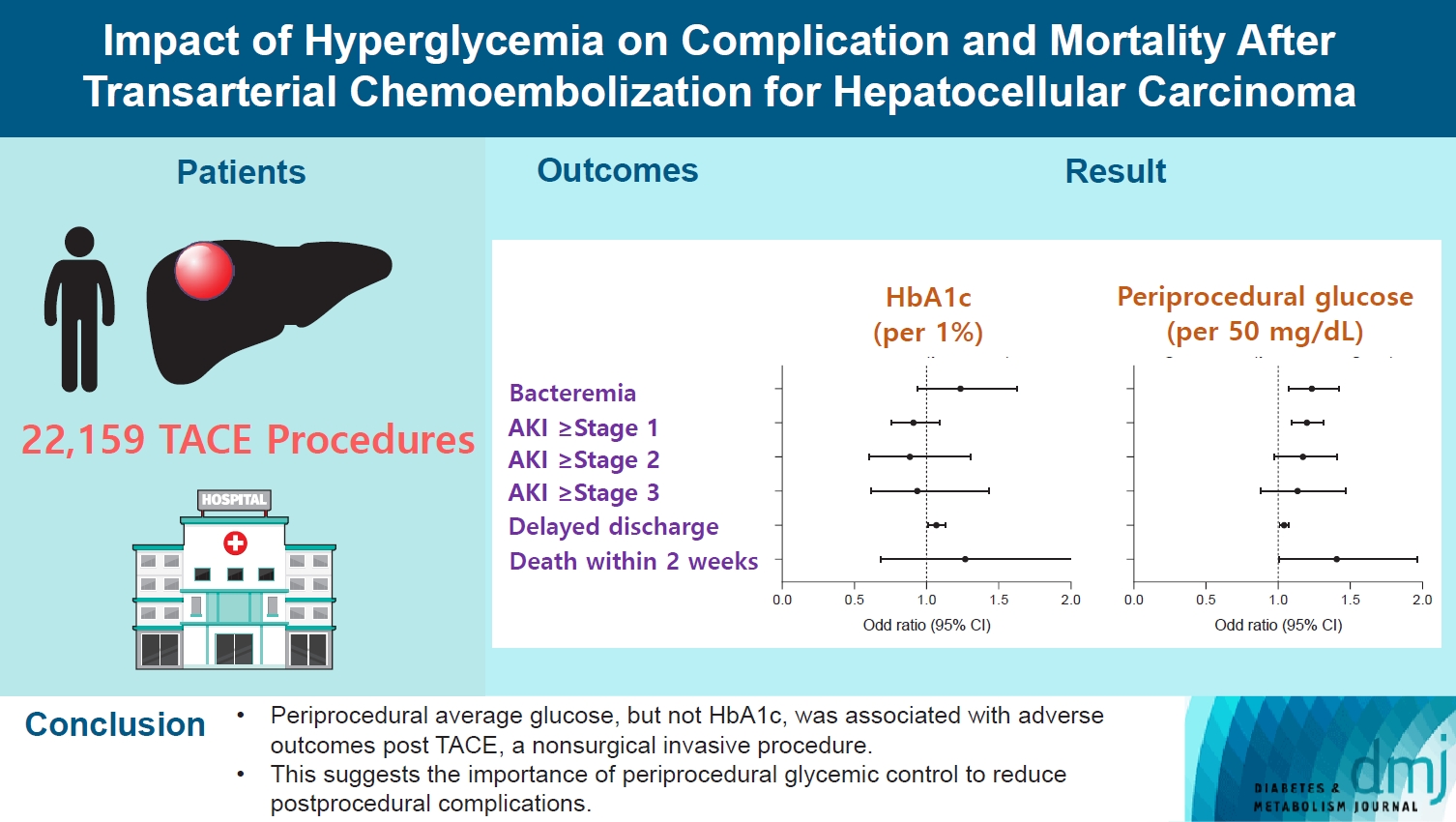
- Impact of Hyperglycemia on Complication and Mortality after Transarterial Chemoembolization for Hepatocellular Carcinoma
- Sun Joon Moon, Chang Ho Ahn, Yun Bin Lee, Young Min Cho
- Diabetes Metab J. 2024;48(2):302-311. Published online January 3, 2024
- DOI: https://doi.org/10.4093/dmj.2022.0255
- 735 View
- 110 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Current guidelines regarding periprocedural glycemic control to prevent complications after nonsurgical invasive procedures are insufficient. Transarterial chemoembolization (TACE) is a widely used treatment for unresectable hepatocellular carcinoma. We aimed to investigate the association between diabetes mellitus (DM) per se and the degree of hyperglycemia with postprocedural complications after TACE.
Methods
A total of 22,159 TACE procedures performed at Seoul National University Hospital from 2005 to 2018 were retrospectively analyzed. The associations between DM, preprocedural glycosylated hemoglobin (HbA1c), and periprocedural average glucose with postprocedural adverse outcomes were evaluated. The primary outcome was occurrence of postprocedural bacteremia. Secondary outcomes were acute kidney injury (AKI), delayed discharge and death within 14 days. Periprocedural glucose was averaged over 3 days: the day of, before, and after the TACE procedures. Propensity score matching was applied for procedures between patients with or without DM.
Results
Periprocedural average glucose was significantly associated with bacteremia (adjusted odds ratio per 50 mg/dL of glucose, 1.233; 95% confidence interval, 1.071 to 1.420; P=0.004), AKI, delayed discharge, and death within 14 days. DM per se was only associated with bacteremia and AKI. Preprocedural HbA1c was associated with delayed discharge. Average glucose levels above 202 and 181 mg/dL were associated with a significantly higher risk of bacteremia and AKI, respectively, than glucose levels of 126 mg/dL or lower.
Conclusion
Periprocedural average glucose, but not HbA1c, was associated with adverse outcomes after TACE, which is a nonsurgical invasive procedure. This suggests the importance of periprocedural glycemic control to reduce postprocedural complications.
- Basic Research
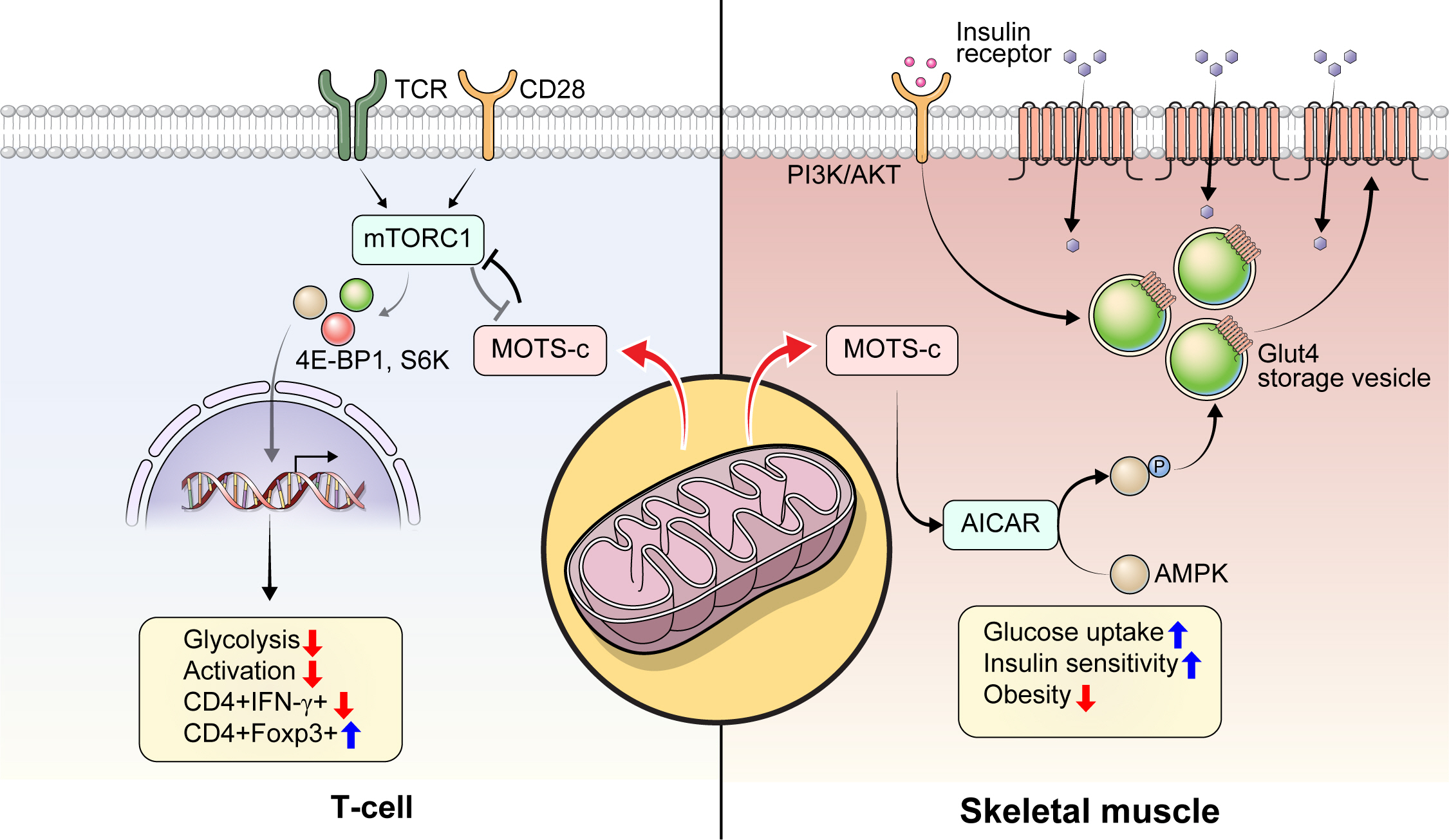
- Mitochondrial-Encoded Peptide MOTS-c, Diabetes, and Aging-Related Diseases
- Byung Soo Kong, Changhan Lee, Young Min Cho
- Diabetes Metab J. 2023;47(3):315-324. Published online February 24, 2023
- DOI: https://doi.org/10.4093/dmj.2022.0333
- 5,722 View
- 284 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Mitochondria are complex metabolic organelles with manifold pathophysiological implications in diabetes. Currently published mitochondrial-encoded peptides, which are expressed from the mitochondrial open reading frame of the 12S ribosomal RNA type-c (MOTS-c), 16S rRNA (humanin and short humanin like peptide 1-6 [SHLP1-6]), or small human mitochondrial open reading frame over serine tRNA (SHMOOSE) are associated with regulation of cellular metabolism and insulin action in age-related diseases, such as type 2 diabetes mellitus. This review focuses mainly on recent advances in MOTS-c research with regards to diabetes, including both type 1 and type 2. The emerging understanding of MOTS-c in diabetes may provide insight into the development of new therapies for diabetes and other age or senescence-related diseases.
-
Citations
Citations to this article as recorded by- Mitochondrial-derived peptides: Antidiabetic functions and evolutionary perspectives
Satadeepa Kal, Sumana Mahata, Suborno Jati, Sushil K. Mahata
Peptides.2024; 172: 171147. CrossRef - Mitochondrial Stress and Mitokines: Therapeutic Perspectives for the Treatment of Metabolic Diseases
Benyuan Zhang, Joon Young Chang, Min Hee Lee, Sang-Hyeon Ju, Hyon-Seung Yi, Minho Shong
Diabetes & Metabolism Journal.2024; 48(1): 1. CrossRef - Mitochondrial bioenergetics, metabolism, and beyond in pancreatic β-cells and diabetes
Alejandra María Rivera Nieves, Brian Michael Wauford, Accalia Fu
Frontiers in Molecular Biosciences.2024;[Epub] CrossRef
- Mitochondrial-derived peptides: Antidiabetic functions and evolutionary perspectives
- Drug/Regimen
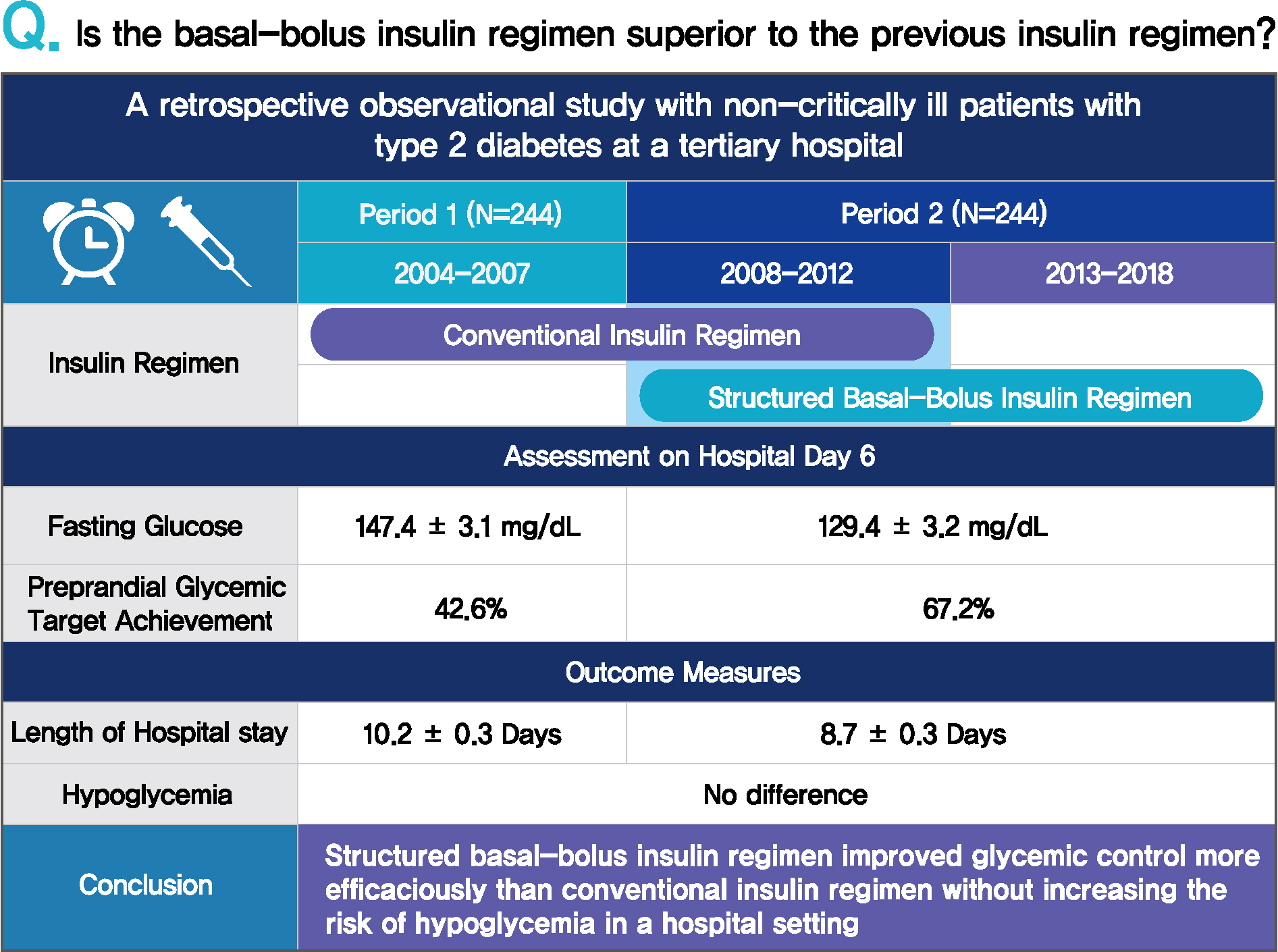
- Comparison of Prevailing Insulin Regimens at Different Time Periods in Hospitalized Patients: A Real-World Experience from a Tertiary Hospital
- Sun Joon Moon, Hun Jee Choe, Soo Heon Kwak, Hye Seung Jung, Kyong Soo Park, Young Min Cho
- Diabetes Metab J. 2022;46(3):439-450. Published online October 20, 2021
- DOI: https://doi.org/10.4093/dmj.2021.0065
- 65,535 View
- 268 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Prevailing insulin regimens for glycemic control in hospitalized patients have changed over time. We aimed to determine whether the current basal-bolus insulin (BBI) regimen is superior to the previous insulin regimen, mainly comprising split-mixed insulin therapy.
Methods
This was a single tertiary center, retrospective observational study that included non-critically ill patients with type 2 diabetes mellitus who were treated with split-mixed insulin regimens from 2004 to 2007 (period 1) and with BBI from 2008 to 2018 (period 2). Patients from each period were analyzed after propensity score matching. The mean difference in glucose levels and the achievement of fasting and preprandial glycemic targets by day 6 of admission were assessed. The total daily insulin dose, incidence of hypoglycemia, and length of hospital stay were also evaluated.
Results
Among 244 patients from each period, both fasting glucose (estimated mean±standard error, 147.4±3.1 mg/dL vs. 129.4±3.2 mg/dL, P<0.001, day 6) and preprandial glucose (177.7±2.8 mg/dL vs. 152.8±2.8 mg/dL, P<0.001, day 6) were lower in period 2 than in period 1. By day 6 of hospital admission, 42.6% and 67.2% of patients achieved a preprandial glycemic target of <140 mg/dL in periods 1 and 2, respectively (relative risk, 2.00; 95% confidence interval, 1.54 to 2.59), without an increased incidence of hypoglycemia. Length of stay was shorter in period 2 (10.23±0.26 days vs. 8.70±0.26 days, P<0.001).
Conclusion
BBI improved glycemic control in a more efficacious manner than a split-mixed insulin regimen without increasing the risk of hypoglycemia in a hospital setting.
- Drug/Regimen
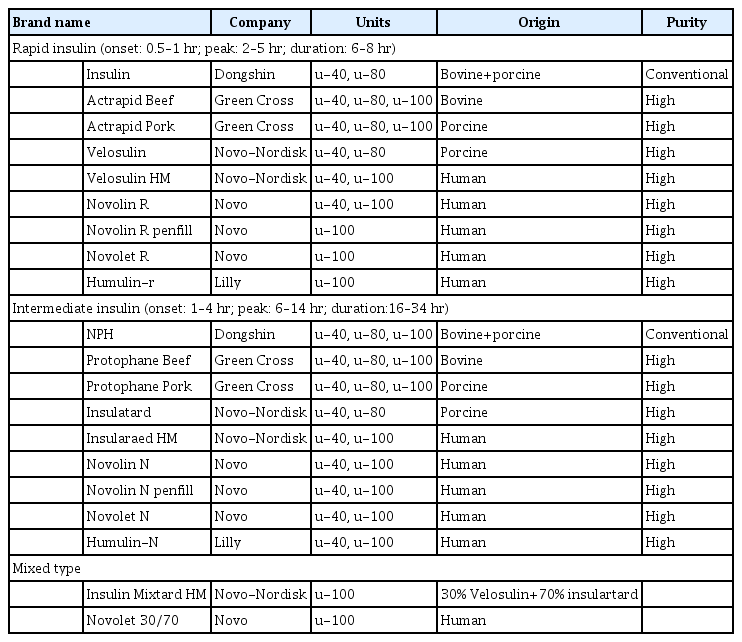
- The History of Insulin Therapy in Korea
- Jun Sung Moon, Jong Chul Won, Young Min Cho
- Diabetes Metab J. 2021;45(5):623-628. Published online September 30, 2021
- DOI: https://doi.org/10.4093/dmj.2021.0171
- 4,043 View
- 136 Download
- 1 Web of Science
- 1 Crossref
- Drug/Regimen
- Efficacy and Safety of Self-Titration Algorithms of Insulin Glargine 300 units/mL in Individuals with Uncontrolled Type 2 Diabetes Mellitus (The Korean TITRATION Study): A Randomized Controlled Trial
- Jae Hyun Bae, Chang Ho Ahn, Ye Seul Yang, Sun Joon Moon, Soo Heon Kwak, Hye Seung Jung, Kyong Soo Park, Young Min Cho
- Diabetes Metab J. 2022;46(1):71-80. Published online June 16, 2021
- DOI: https://doi.org/10.4093/dmj.2020.0274

- 7,964 View
- 434 Download
- 1 Web of Science
- 3 Crossref
-
 Graphical Abstract
Graphical Abstract
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub 
- Background
To compare the efficacy and safety of two insulin self-titration algorithms, Implementing New Strategies with Insulin Glargine for Hyperglycemia Treatment (INSIGHT) and EDITION, for insulin glargine 300 units/mL (Gla-300) in Korean individuals with uncontrolled type 2 diabetes mellitus (T2DM).
Methods
In a 12-week, randomized, open-label trial, individuals with uncontrolled T2DM requiring basal insulin were randomized to either the INSIGHT (adjusted by 1 unit/day) or EDITION (adjusted by 3 units/week) algorithm to achieve a fasting self-monitoring of blood glucose (SMBG) in the range of 4.4 to 5.6 mmol/L. The primary outcome was the proportion of individuals achieving a fasting SMBG ≤5.6 mmol/L without noct urnal hypoglycemia at week 12.
Results
Of 129 individuals (age, 64.1±9.5 years; 66 [51.2%] women), 65 and 64 were randomized to the INSIGHT and EDITION algorithms, respectively. The primary outcome of achievement was comparable between the two groups (24.6% vs. 23.4%, P=0.876). Compared with the EDITION group, the INSIGHT group had a greater reduction in 7-point SMBG but a similar decrease in fasting plasma glucose and glycosylated hemoglobin. The increment of total daily insulin dose was significantly higher in the INSIGHT group than in the EDITION group (between-group difference: 5.8±2.7 units/day, P=0.033). However, body weight was significantly increased only in the EDITION group (0.6±2.4 kg, P=0.038). There was no difference in the occurrence of hypoglycemia between the two groups. Patient satisfaction was significantly increased in the INSIGHT group (P=0.014).
Conclusion
The self-titration of Gla-300 using the INSIGHT algorithm was effective and safe compared with that using the EDITION algorithm in Korean individuals with uncontrolled T2DM (ClinicalTrials.gov number: NCT03406663). -
Citations
Citations to this article as recorded by- Basal insulin titration algorithms in patients with type 2 diabetes: the simplest is the best (?)
V.I. Katerenchuk
INTERNATIONAL JOURNAL OF ENDOCRINOLOGY (Ukraine).2023; 19(1): 72. CrossRef - Issues of insulin therapy for type 2 diabetes and ways to solve them
V.I. Katerenchuk, A.V. Katerenchuk
INTERNATIONAL JOURNAL OF ENDOCRINOLOGY (Ukraine).2023; 19(3): 240. CrossRef - Time for Using Machine Learning for Dose Guidance in Titration of People With Type 2 Diabetes? A Systematic Review of Basal Insulin Dose Guidance
Camilla Heisel Nyholm Thomsen, Stine Hangaard, Thomas Kronborg, Peter Vestergaard, Ole Hejlesen, Morten Hasselstrøm Jensen
Journal of Diabetes Science and Technology.2022; : 193229682211459. CrossRef
- Basal insulin titration algorithms in patients with type 2 diabetes: the simplest is the best (?)
- Response: Premeal Consumption of a Protein-Enriched, Dietary Fiber-Fortified Bar Decreases Total Energy Intake in Healthy Individuals (
Diabetes Metab J 2019;43:879–92) - Chang Ho Ahn, Jae Hyun Bae, Young Min Cho
- Diabetes Metab J. 2020;44(1):207-208. Published online February 21, 2020
- DOI: https://doi.org/10.4093/dmj.2020.0026
- [Original]
- 3,340 View
- 49 Download
- Drug/Regimen
-
- Glucagon-Like Peptide-1 Receptor Agonist Differentially Affects Brain Activation in Response to Visual Food Cues in Lean and Obese Individuals with Type 2 Diabetes Mellitus
- Jae Hyun Bae, Hyung Jin Choi, Kang Ik Kevin Cho, Lee Kyung Kim, Jun Soo Kwon, Young Min Cho
- Diabetes Metab J. 2020;44(2):248-259. Published online November 4, 2019
- DOI: https://doi.org/10.4093/dmj.2019.0018
- 7,373 View
- 222 Download
- 5 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader Background To investigate the effects of a glucagon-like peptide-1 receptor agonist on functional brain activation in lean and obese individuals with type 2 diabetes mellitus (T2DM) in response to visual food cues.
Methods In a randomized, single-blinded, crossover study, 15 lean and 14 obese individuals with T2DM were administered lixisenatide or normal saline subcutaneously with a 1-week washout period. We evaluated brain activation in response to pictures of high-calorie food, low-calorie food, and nonfood using functional magnetic resonance imaging and measured appetite and caloric intake in participants who were given access to an
ad libitum buffet.Results Obese individuals with T2DM showed significantly greater activation of the hypothalamus, pineal gland, parietal cortex (high-calorie food vs. low-calorie food,
P <0.05), orbitofrontal cortex (high-calorie food vs. nonfood,P <0.05), and visual cortex (food vs. nonfood,P <0.05) than lean individuals with T2DM. Lixisenatide injection significantly reduced the functional activation of the fusiform gyrus and lateral ventricle in obese individuals with T2DM compared with that in lean individuals with T2DM (nonfood vs. high-calorie food,P <0.05). In addition, in individuals who decreased their caloric intake after lixisenatide injection, there were significant interaction effects between group and treatment in the posterior cingulate, medial frontal cortex (high-calorie food vs. low-calorie food,P <0.05), hypothalamus, orbitofrontal cortex, and temporal lobe (food vs. nonfood,P <0.05).Conclusion Brain responses to visual food cues were different in lean and obese individuals with T2DM. In addition, acute administration of lixisenatide differentially affected functional brain activation in these individuals, especially in those who decreased their caloric intake after lixisenatide injection.
-
Citations
Citations to this article as recorded by- Altered Metabolic Phenotypes and Hypothalamic Neuronal Activity Triggered by Sodium-Glucose Cotransporter 2 Inhibition (Diabetes Metab J 2023;47:784-95)
Jae Hyun Bae
Diabetes & Metabolism Journal.2024; 48(1): 157. CrossRef - Diabetes remission and relapse following an intensive metabolic intervention combining insulin glargine/lixisenatide, metformin and lifestyle approaches: Results of a randomised controlled trial
Natalia McInnes, Stephanie Hall, Heather A. Lochnan, Stewart B. Harris, Zubin Punthakee, Ronald J. Sigal, Irene Hramiak, Mohammed Azharuddin, Joanne F. Liutkus, Jean‐François Yale, Farah Sultan, Ada Smith, Rose E. Otto, Diana Sherifali, Yan Yun Liu, Hertz
Diabetes, Obesity and Metabolism.2023; 25(11): 3347. CrossRef - Glucagon-like peptide-1 analog therapy in rare genetic diseases: monogenic obesity, monogenic diabetes, and spinal muscular atrophy
Hussein Zaitoon, Ronit Lubetzky, Achiya Z. Amir, Hadar Moran-Lev, Liora Sagi, Michal Yacobi-Bach, Ophir Borger, Efrat Chorna, Yael Lebenthal, Avivit Brener
Acta Diabetologica.2023; 60(8): 1099. CrossRef - What can functional brain imaging teach us about remission of type 2 diabetes?
Dhruti Hirani, Shahd Alabdulkader, Alexander. D. Miras, Victoria Salem
Diabetic Medicine.2023;[Epub] CrossRef - Fasting oxyntomodulin, glicentin, and gastric inhibitory polypeptide levels are associated with activation of reward‐ and attention‐related brain centres in response to visual food cues in adults with obesity: A cross‐sectional functional MRI study
Nikolaos Perakakis, Olivia M. Farr, Christos S. Mantzoros
Diabetes, Obesity and Metabolism.2021; 23(5): 1202. CrossRef - Aberrant Brain Functional Connectivity Strength and Effective Connectivity in Patients with Type 2 Diabetes Mellitus
Xi Guo, Su Wang, Yu-Chen Chen, Heng-Le Wei, Gang-Ping Zhou, Yu-Sheng Yu, Xindao Yin, Kun Wang, Hong Zhang, Eusebio Chiefari
Journal of Diabetes Research.2021; 2021: 1. CrossRef
- Altered Metabolic Phenotypes and Hypothalamic Neuronal Activity Triggered by Sodium-Glucose Cotransporter 2 Inhibition (Diabetes Metab J 2023;47:784-95)
- Obesity and Metabolic Syndrome
- Premeal Consumption of a Protein-Enriched, Dietary Fiber-Fortified Bar Decreases Total Energy Intake in Healthy Individuals
- Chang Ho Ahn, Jae Hyun Bae, Young Min Cho
- Diabetes Metab J. 2019;43(6):879-892. Published online June 25, 2019
- DOI: https://doi.org/10.4093/dmj.2018.0202
- 4,982 View
- 84 Download
- 3 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader Background A premeal load of protein can increase satiety and reduce energy intake. Dietary fiber also conveys metabolic benefits by modulating energy intake. We made a protein-enriched, dietary fiber-fortified bar (PFB) and aimed to investigate its effects on food intake and gut hormone secretion in healthy individuals.
Methods Twenty subjects with normal glucose tolerance were enrolled. On three separate visits, the subjects received, in a randomized order, one of the following: a PFB containing 73 kcal with 10.7 g of protein and 12.7 g of dietary fiber; a usual bar (UB) containing the same calories as the PFB but only 0.9 g of protein and no dietary fiber; or water (control). After 15 minutes, the subjects had
ad libitum intake of a test meal. Food consumption, appetite, and plasma gut hormone levels were measured.Results Total energy intake, including the bar and the test meal, was significantly reduced with the PFB preload compared to the water (904.4±534.9 kcal vs. 1,075.0±508.0 kcal,
P =0.016). With the UB preload, only the intake of the test meal was reduced (P =0.044) but not the total energy intake (P =0.471) than the water. Fullness was also significantly increased after the PFB. In addition, postprandial glucose levels decreased and glucagon-like peptide-1 levels increased with the PFB compared with both the UB and water.Conclusion In healthy individuals, a premeal supplementation of PFB reduced total energy intake and decreased postprandial glucose excursion. This finding necessitates long-term studies regarding clinical use in obesity.
-
Citations
Citations to this article as recorded by- Citrus pectin protects mice from burn injury by modulating intestinal microbiota, GLP-1 secretion and immune response
Ji-Wei Hao, Hong-Sheng Liu, Ling-Ying Liu, Qing-Hong Zhang
International Immunopharmacology.2024; 131: 111912. CrossRef - Effect of Two Different Meal Compositions on 1-hour Plasma Ghrelin Levels in Young Men
Brinnell Annette Caszo, Sangeetha Shyam, Purushotham Krishnappa, Justin Vijay Gnanou
Malaysian Journal of Medicine and Health Sciences.2023; 19(5): 185. CrossRef - Intake of Fibre-Associated Foods and Texture Preferences in Relation to Weight Status Among 9–12 Years Old Children in 6 European Countries
Marlies Hörmann-Wallner, Raphaela Krause, Begoña Alfaro, Hannah Jilani, Monica Laureati, Valérie L. Almli, Mari Sandell, Pernilla Sandvik, Gertrude G. Zeinstra, Lisa Methven
Frontiers in Nutrition.2021;[Epub] CrossRef - Response: Premeal Consumption of a Protein-Enriched, Dietary Fiber-Fortified Bar Decreases Total Energy Intake in Healthy Individuals (Diabetes Metab J 2019;43:879–92)
Chang Ho Ahn, Jae Hyun Bae, Young Min Cho
Diabetes & Metabolism Journal.2020; 44(1): 207. CrossRef - Letter: Premeal Consumption of a Protein-Enriched, Dietary Fiber-Fortified Bar Decreases Total Energy Intake in Healthy Individuals (Diabetes Metab J 2019;43:879–92)
Mi-kyung Kim
Diabetes & Metabolism Journal.2020; 44(1): 203. CrossRef - Spent coffee (Coffea arabicaL.) grounds promote satiety and attenuate energy intake: A pilot study
Rocio Campos‐Vega, Andrea Arreguín‐Campos, Miguel A. Cruz‐Medrano, María Dolores Castillo Bilbao
Journal of Food Biochemistry.2020;[Epub] CrossRef
- Citrus pectin protects mice from burn injury by modulating intestinal microbiota, GLP-1 secretion and immune response
- Clinical Diabetes & Therapeutics
- Effectiveness and Safety of Adding Basal Insulin Glargine in Patients with Type 2 Diabetes Mellitus Exhibiting Inadequate Response to Metformin and DPP-4 Inhibitors with or without Sulfonylurea
- Yu Mi Kang, Chang Hee Jung, Seung-Hwan Lee, Sang-Wook Kim, Kee-Ho Song, Sin Gon Kim, Jae Hyeon Kim, Young Min Cho, Tae Sun Park, Bon Jeong Ku, Gwanpyo Koh, Dol Mi Kim, Byung-Wan Lee, Joong-Yeol Park
- Diabetes Metab J. 2019;43(4):432-446. Published online June 19, 2019
- DOI: https://doi.org/10.4093/dmj.2018.0092
- 5,554 View
- 89 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader Background We aimed to investigate the effectiveness and safety of adding basal insulin to initiating dipeptidyl peptidase-4 (DPP-4) inhibitor and metformin and/or sulfonylurea (SU) in achieving the target glycosylated hemoglobin (HbA1c) in patients with type 2 diabetes mellitus (T2DM).
Methods This was a single-arm, multicenter, 24-week, open-label, phase 4 study in patients with inadequately controlled (HbA1c ≥7.5%) T2DM despite the use of DPP-4 inhibitor and metformin. A total of 108 patients received insulin glargine while continuing oral antidiabetic drugs (OADs). The primary efficacy endpoint was the percentage of subjects achieving HbA1c ≤7.0%. Other glycemic profiles were also evaluated, and the safety endpoints were adverse events (AEs) and hypoglycemia.
Results The median HbA1c at baseline (8.9%; range, 7.5% to 11.1%) decreased to 7.6% (5.5% to 11.7%) at 24 weeks. Overall, 31.7% subjects (
n =33) achieved the target HbA1c level of ≤7.0%. The mean differences in body weight and fasting plasma glucose were 1.2±3.4 kg and 56.0±49.8 mg/dL, respectively. Hypoglycemia was reported in 36 subjects (33.3%, 112 episodes), all of which were fully recovered. There was no serious AE attributed to insulin glargine. Body weight change was significantly different between SU users and nonusers (1.5±2.5 kg vs. −0.9±6.0 kg,P =0.011).Conclusion The combination add-on therapy of insulin glargine, on metformin and DPP-4 inhibitors with or without SU was safe and efficient in reducing HbA1c levels and thus, is a preferable option in managing T2DM patients exhibiting dysglycemia despite the use of OADs.
-
Citations
Citations to this article as recorded by- Glycaemic control with add‐on thiazolidinedione or a sodium‐glucose co‐transporter‐2 inhibitor in patients with type 2 diabetes after the failure of an oral triple antidiabetic regimen: A 24‐week, randomized controlled trial
Jaehyun Bae, Ji Hye Huh, Minyoung Lee, Yong‐Ho Lee, Byung‐Wan Lee
Diabetes, Obesity and Metabolism.2021; 23(2): 609. CrossRef - Beneficial effect of anti-diabetic drugs for nonalcoholic fatty liver disease
Kyung-Soo Kim, Byung-Wan Lee
Clinical and Molecular Hepatology.2020; 26(4): 430. CrossRef
- Glycaemic control with add‐on thiazolidinedione or a sodium‐glucose co‐transporter‐2 inhibitor in patients with type 2 diabetes after the failure of an oral triple antidiabetic regimen: A 24‐week, randomized controlled trial
- Others
- Application of the Oral Minimal Model to Korean Subjects with Normal Glucose Tolerance and Type 2 Diabetes Mellitus
- Min Hyuk Lim, Tae Jung Oh, Karam Choi, Jung Chan Lee, Young Min Cho, Sungwan Kim
- Diabetes Metab J. 2016;40(4):308-317. Published online June 2, 2016
- DOI: https://doi.org/10.4093/dmj.2016.40.4.308
- 4,837 View
- 74 Download
- 2 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background The oral minimal model is a simple, useful tool for the assessment of β-cell function and insulin sensitivity across the spectrum of glucose tolerance, including normal glucose tolerance (NGT), prediabetes, and type 2 diabetes mellitus (T2DM) in humans.
Methods Plasma glucose, insulin, and C-peptide levels were measured during a 180-minute, 75-g oral glucose tolerance test in 24 Korean subjects with NGT (
n =10) and T2DM (n =14). The parameters in the computational model were estimated, and the indexes for insulin sensitivity and β-cell function were compared between the NGT and T2DM groups.Results The insulin sensitivity index was lower in the T2DM group than the NGT group. The basal index of β-cell responsivity, basal hepatic insulin extraction ratio, and post-glucose challenge hepatic insulin extraction ratio were not different between the NGT and T2DM groups. The dynamic, static, and total β-cell responsivity indexes were significantly lower in the T2DM group than the NGT group. The dynamic, static, and total disposition indexes were also significantly lower in the T2DM group than the NGT group.
Conclusion The oral minimal model can be reproducibly applied to evaluate β-cell function and insulin sensitivity in Koreans.
-
Citations
Citations to this article as recorded by- Fimasartan increases glucose‐stimulated insulin secretion in patients with type 2 diabetes and hypertension compared with amlodipine
Ye Seul Yang, Min Hyuk Lim, Seong Ok Lee, Eun Roh, Chang Ho Ahn, Soo Heon Kwak, Young Min Cho, Sungwan Kim, Andrea Mari, Kyong Soo Park, Hye Seung Jung
Diabetes, Obesity and Metabolism.2018; 20(7): 1670. CrossRef - The Cut-off Values of Triglycerides and Glucose Index for Metabolic Syndrome in American and Korean Adolescents
Shinje Moon, Joon-Sung Park, Youhern Ahn
Journal of Korean Medical Science.2017; 32(3): 427. CrossRef
- Fimasartan increases glucose‐stimulated insulin secretion in patients with type 2 diabetes and hypertension compared with amlodipine
- Clinical Care/Education
- Feasibility of a Patient-Centered, Smartphone-Based, Diabetes Care System: A Pilot Study
- Eun Ky Kim, Soo Heon Kwak, Seungsu Baek, Seung Lyeol Lee, Hak Chul Jang, Kyong Soo Park, Young Min Cho
- Diabetes Metab J. 2016;40(3):192-201. Published online April 8, 2016
- DOI: https://doi.org/10.4093/dmj.2016.40.3.192
- 5,093 View
- 53 Download
- 20 Web of Science
- 25 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background We developed a patient-centered, smartphone-based, diabetes care system (PSDCS). This study aims to test the feasibility of glycosylated hemoglobin (HbA1c) reduction with the PSDCS.
Methods This study was a single-arm pilot study. The participants with type 2 diabetes mellitus were instructed to use the PSDCS, which integrates a Bluetooth-connected glucometer, digital food diary, and wearable physical activity monitoring device. The primary end point was the change in HbA1c from baseline after a 12-week intervention.
Results Twenty-nine patients aged 53.9±9.1 years completed the study. HbA1c and fasting plasma glucose levels decreased significantly from baseline (7.7%±0.7% to 7.1%±0.6%,
P <0.0001; 140.9±39.1 to 120.1±31.0 mg/dL,P =0.0088, respectively). The frequency of glucose monitoring correlated with the magnitude of HbA1c reduction (r =–0.57,P =0.0013). The components of the diabetes self-care activities, including diet, exercise, and glucose monitoring, were significantly improved, particularly in the upper tertile of HbA1c reduction. There were no severe adverse events during the intervention.Conclusion A 12-week application of the PSDCS to patients with inadequately controlled type 2 diabetes resulted in a significant HbA1c reduction with tolerable safety profiles; these findings require confirmation in a future randomized controlled trial.
-
Citations
Citations to this article as recorded by- Telehealth Technologies in Diabetes Self-management and Education
Vidya Sharma, Marie Feldman, Ramaswamy Sharma
Journal of Diabetes Science and Technology.2024; 18(1): 148. CrossRef - App Design Features Important for Diabetes Self-management as Determined by the Self-Determination Theory on Motivation: Content Analysis of Survey Responses From Adults Requiring Insulin Therapy
Helen N C Fu, Jean F Wyman, Cynthia J Peden-McAlpine, Claire Burke Draucker, Titus Schleyer, Terrence J Adam
JMIR Diabetes.2023; 8: e38592. CrossRef - The Clinical Impact of Flash Glucose Monitoring—a Digital Health App and Smartwatch Technology in Patients With Type 2 Diabetes: Scoping Review
Sergio Diez Alvarez, Antoni Fellas, Derek Santos, Dean Sculley, Katie Wynne, Shamasunder Acharya, Pooshan Navathe, Xavier Girones, Andrea Coda
JMIR Diabetes.2023; 8: e42389. CrossRef - User Retention and Engagement in the Digital-Based Diabetes Education and Self-Management for Ongoing and Newly Diagnosed (myDESMOND) Program: Descriptive Longitudinal Study
Mary M Barker, Radhika Chauhan, Melanie J Davies, Christopher Brough, Alison Northern, Bernie Stribling, Sally Schreder, Kamlesh Khunti, Michelle Hadjiconstantinou
JMIR Diabetes.2023; 8: e44943. CrossRef - New Digital Health Technologies for Insulin Initiation and Optimization for People With Type 2 Diabetes
David Kerr, Steven Edelman, Giacomo Vespasiani, Kamlesh Khunti
Endocrine Practice.2022; 28(8): 811. CrossRef - Effects of Patient-Driven Lifestyle Modification Using Intermittently Scanned Continuous Glucose Monitoring in Patients With Type 2 Diabetes: Results From the Randomized Open-label PDF Study
Hun Jee Choe, Eun-Jung Rhee, Jong Chul Won, Kyong Soo Park, Won-Young Lee, Young Min Cho
Diabetes Care.2022; 45(10): 2224. CrossRef - Assessing the Acceptability and Effectiveness of Mobile-Based Physical Activity Interventions for Midlife Women During Menopause: Systematic Review of the Literature
Ghada AlSwayied, Haoyue Guo, Tasmin Rookes, Rachael Frost, Fiona L Hamilton
JMIR mHealth and uHealth.2022; 10(12): e40271. CrossRef - Application of the National Institute for Health and Care Excellence Evidence Standards Framework for Digital Health Technologies in Assessing Mobile-Delivered Technologies for the Self-Management of Type 2 Diabetes Mellitus: Scoping Review
Jessica R Forsyth, Hannah Chase, Nia W Roberts, Laura C Armitage, Andrew J Farmer
JMIR Diabetes.2021; 6(1): e23687. CrossRef - Mobile Healthcare System Provided by Primary Care Physicians Improves Quality of Diabetes Care
Tae Jung Oh, Jie-Eun Lee, Seok Kim, Sooyoung Yoo, Hak Chul Jang
CardioMetabolic Syndrome Journal.2021; 1(1): 88. CrossRef - Self-Care IoT Platform for Diabetic Mellitus
Jai-Chang Park, Seongbeom Kim, Je-Hoon Lee
Applied Sciences.2021; 11(5): 2006. CrossRef - Diabetes clinic reinvented: will technology change the future of diabetes care?
Marwa Al-Badri, Osama Hamdy
Therapeutic Advances in Endocrinology and Metabolism.2021; 12: 204201882199536. CrossRef - Analysis of Effectiveness and Psychological Techniques Implemented in mHealth Solutions for Middle-Aged and Elderly Adults with Type 2 Diabetes: A Narrative Review of the Literature
Julia Vázquez-de Sebastián, Andreea Ciudin, Carmina Castellano-Tejedor
Journal of Clinical Medicine.2021; 10(12): 2701. CrossRef - Therapeutic Exercise Platform for Type-2 Diabetic Mellitus
Je-Hoon Lee, Jai-Chang Park, Seong-Beom Kim
Electronics.2021; 10(15): 1820. CrossRef - Accuracy comparison study of new smartphone-based semen analyzer versus laboratory sperm quality analyzer
Min Jung Park, Mi Young Lim, Hyun Jun Park, Nam Cheol Park
Investigative and Clinical Urology.2021; 62(6): 672. CrossRef - User Retention and Engagement With a Mobile App Intervention to Support Self-Management in Australians With Type 1 or Type 2 Diabetes (My Care Hub): Mixed Methods Study
Mary D Adu, Usman H Malabu, Aduli EO Malau-Aduli, Aaron Drovandi, Bunmi S Malau-Aduli
JMIR mHealth and uHealth.2020; 8(6): e17802. CrossRef - The role of telehealth counselling with mobile self-monitoring on blood pressure reduction among overseas Koreans with high blood pressure in Vietnam
Hyang Yuol Lee, Ju Young Kim, Ki Young Na, Hwa Yeon Park, Jinah Han, Yuliya Pak, Bola Nam, Chae Hyun Pae, Jisun Lee, Tae Ho Lim, Donghun Lee
Journal of Telemedicine and Telecare.2019; 25(4): 241. CrossRef - The Effect of a Smartphone-Based, Patient-Centered Diabetes Care System in Patients With Type 2 Diabetes: A Randomized, Controlled Trial for 24 Weeks
Eun Ky Kim, Soo Heon Kwak, Hye Seung Jung, Bo Kyung Koo, Min Kyong Moon, Soo Lim, Hak Chul Jang, Kyong Soo Park, Young Min Cho
Diabetes Care.2019; 42(1): 3. CrossRef - Patient-Driven Diabetes Care of the Future in the Technology Era
Sahar Ashrafzadeh, Osama Hamdy
Cell Metabolism.2019; 29(3): 564. CrossRef - Peripartum Management of Gestational Diabetes Using a Digital Health Care Service: A Pilot, Randomized Controlled Study
Ji-Hee Sung, Da Young Lee, Kyoung Pil Min, Cheol-Young Park
Clinical Therapeutics.2019; 41(11): 2426. CrossRef - The Effects of Dietary Mobile Apps on Nutritional Outcomes in Adults with Chronic Diseases: A Systematic Review and Meta-Analysis
Cosette Fakih El Khoury, Mirey Karavetian, Ruud J.G. Halfens, Rik Crutzen, Lama Khoja, Jos M.G.A. Schols
Journal of the Academy of Nutrition and Dietetics.2019; 119(4): 626. CrossRef - Diabetes Mellitus m-Health Applications: A Systematic Review of Features and Fundamentals
Ericles Andrei Bellei, Daiana Biduski, Nathália Pinto Cechetti, Ana Carolina Bertoletti De Marchi
Telemedicine and e-Health.2018; 24(11): 839. CrossRef - Multifunctional Wearable System that Integrates Sweat‐Based Sensing and Vital‐Sign Monitoring to Estimate Pre‐/Post‐Exercise Glucose Levels
Yongseok Joseph Hong, Hyunjae Lee, Jaemin Kim, Minha Lee, Hyung Jin Choi, Taeghwan Hyeon, Dae‐Hyeong Kim
Advanced Functional Materials.2018;[Epub] CrossRef - Smart Devices for Older Adults Managing Chronic Disease: A Scoping Review
Ben YB Kim, Joon Lee
JMIR mHealth and uHealth.2017; 5(5): e69. CrossRef - Usability and clinical efficacy of diabetes mobile applications for adults with type 2 diabetes: A systematic review
Helen Fu, Siobhan K. McMahon, Cynthia R. Gross, Terrence J. Adam, Jean F. Wyman
Diabetes Research and Clinical Practice.2017; 131: 70. CrossRef - Novel device for male infertility screening with single-ball lens microscope and smartphone
Yoshitomo Kobori, Peter Pfanner, Gail S. Prins, Craig Niederberger
Fertility and Sterility.2016; 106(3): 574. CrossRef
- Telehealth Technologies in Diabetes Self-management and Education
- Clinical Care/Education
- Clinical Characteristics and Metabolic Predictors of Rapid Responders to Dipeptidyl Peptidase-4 Inhibitor as an Add-on Therapy to Sulfonylurea and Metformin
- Ye An Kim, Won Sang Yoo, Eun Shil Hong, Eu Jeong Ku, Kyeong Seon Park, Soo Lim, Young Min Cho, Kyong Soo Park, Hak Chul Jang, Sung Hee Choi
- Diabetes Metab J. 2015;39(6):489-497. Published online November 27, 2015
- DOI: https://doi.org/10.4093/dmj.2015.39.6.489
- 3,502 View
- 39 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Dipeptidyl peptidase-4 (DPP-4) inhibitor add-on therapy is a new option for patients with inadequately controlled type 2 diabetes who are taking combined metformin and sulfonylurea (SU). We evaluated the efficacy and safety of this triple therapy and the characteristics of rapid responders and hypoglycemia-prone patients.
Methods We included 807 patients with type 2 diabetes who were prescribed a newly added DPP-4 inhibitor to ongoing metformin and SU in 2009 to 2011. Glycemia and other metabolic parameters at baseline, 12, 24, and 52 weeks, as well as episodes of hypoglycemia were analyzed. Rapid responders were defined as patients with ≥25% reduction in glycosylated hemoglobin (HbA1c) within 12 weeks.
Results At baseline, while on the submaximal metformin and SU combination, the mean HbA1c level was 8.4%. Twelve weeks after initiation of DPP-4 inhibitor add-on, 269 patients (34.4%) achieved an HbA1c level ≤7%. Sixty-six patients (8.2%, 47 men) were rapid responders. The duration of diabetes was shorter in rapid responders, and their baseline fasting plasma glucose (FPG), HbA1c, C-peptide, and homeostasis model assessment of insulin resistance were significantly higher. Patients who experienced hypoglycemia after taking DPP-4 inhibitor add-on were more likely to be female, to have a lower body weight and lower triglyceride and FPG levels, and to have higher homeostasis model assessment of β-cells.
Conclusion An oral hypoglycemic triple agent combination including a DPP-4 inhibitor was effective in patients with uncontrolled diabetes. Proactive dose reduction of SU should be considered when a DPP-4 inhibitor is added for rapid responders and hypoglycemia-prone patients.
-
Citations
Citations to this article as recorded by- A genetic variant in GLP1R is associated with response to DPP-4 inhibitors in patients with type 2 diabetes
Eugene Han, Hye Sun Park, Obin Kwon, Eun Yeong Choe, Hye Jin Wang, Yong-ho Lee, Sang-Hak Lee, Chul Hoon Kim, Lee-Kyung Kim, Soo Heon Kwak, Kyong Soo Park, Chul Sik Kim, Eun Seok Kang
Medicine.2016; 95(44): e5155. CrossRef
- A genetic variant in GLP1R is associated with response to DPP-4 inhibitors in patients with type 2 diabetes
- Genetics
- Identification of Two Cases of Ciliopathy-Associated Diabetes and Their Mutation Analysis Using Whole Exome Sequencing
- Min Kyeong Kim, Soo Heon Kwak, Shinae Kang, Hye Seung Jung, Young Min Cho, Seong Yeon Kim, Kyong Soo Park
- Diabetes Metab J. 2015;39(5):439-443. Published online October 22, 2015
- DOI: https://doi.org/10.4093/dmj.2015.39.5.439
- 4,470 View
- 48 Download
- 5 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Alström syndrome and Bardet-Biedl syndrome are autosomal recessively inherited ciliopathies with common characteristics of obesity, diabetes, and blindness. Alström syndrome is caused by a mutation in the
ALMS1 gene, and Bardet-Biedl syndrome is caused by mutations inBBS1-16 genes. Herein we report genetically confirmed cases of Alström syndrome and Bardet-Biedl syndrome in Korea using whole exome sequencing.Methods Exome capture was done using SureSelect Human All Exon Kit V4+UTRs (Agilent Technologies). HiSeq2000 system (Illumina) was used for massive parallel sequencing. Sanger sequencing was used for genotype confirmation and familial cosegregation analysis.
Results A 21-year old Korean woman was clinically diagnosed with Alström syndrome. She had diabetes, blindness, obesity, severe insulin resistance, and hearing loss. Whole exome sequencing revealed a nonsense mutation in exon 10 of
ALMS1 (c.8776C>T, p.R2926X) and a seven base-pair deletion resulting in frameshift mutation in exon 8 (c.6410_6416del, p.2137_2139del). A 24-year-old Korean man had Bardet-Biedl syndrome with diabetes, blindness, obesity, and a history of polydactyly. Whole exome sequencing revealed a nonsynonymous mutation in exon 11 of theBBS1 gene (c.1061A>G, p.E354G) and mutation at the normal splicing recognition site of exon 7 of theBBS1 gene (c.519-1G>T).Conclusion We found novel compound heterozygous mutations of Alström syndrome and Bardet-Biedl syndrome using whole exome sequencing. The whole exome sequencing successfully identified novel genetic variants of ciliopathy-associated diabetes.
-
Citations
Citations to this article as recorded by- Genotype–phenotype associations in Alström syndrome: a systematic review and meta-analysis
Brais Bea-Mascato, Diana Valverde
Journal of Medical Genetics.2024; 61(1): 18. CrossRef - Differentiating Monogenic and Syndromic Obesities From Polygenic Obesity: Assessment, Diagnosis, and Management
Angela K. Fitch, Sonali Malhotra, Rushika Conroy
Obesity Pillars.2024; : 100110. CrossRef - Whole exome sequencing identifies rare biallelic ALMS1 missense and stop gain mutations in familial Alström syndrome patients
Naglaa M. Kamal, Ahmed N. Sahly, Babajan Banaganapalli, Omran M. Rashidi, Preetha J. Shetty, Jumana Y. Al-Aama, Noor A. Shaik, Ramu Elango, Omar I. Saadah
Saudi Journal of Biological Sciences.2020; 27(1): 271. CrossRef - Established and emerging strategies to crack the genetic code of obesity
V. Tam, M. Turcotte, D. Meyre
Obesity Reviews.2019; 20(2): 212. CrossRef - Identifying Pathogenic Variants of Monogenic Diabetes Using Targeted Panel Sequencing in an East Asian Population
Seung Shin Park, Se Song Jang, Chang Ho Ahn, Jung Hee Kim, Hye Seung Jung, Young Min Cho, Young Ah Lee, Choong Ho Shin, Jong Hee Chae, Jae Hyun Kim, Sung Hee Choi, Hak C Jang, Jee Cheol Bae, Jong Cheol Won, Sung-Hoon Kim, Jong-Il Kim, Soo Heon Kwak, Kyong
The Journal of Clinical Endocrinology & Metabolism.2019; 104(9): 4188. CrossRef - Whole exome sequencing as a diagnostic tool for patients with ciliopathy-like phenotypes
Sheila Castro-Sánchez, María Álvarez-Satta, Mohamed A. Tohamy, Sergi Beltran, Sophia Derdak, Diana Valverde, Anand Swaroop
PLOS ONE.2017; 12(8): e0183081. CrossRef
- Genotype–phenotype associations in Alström syndrome: a systematic review and meta-analysis
- Response: Normal Glucose Tolerance with a High 1-Hour Postload Plasma Glucose Level Exhibits Decreased β-Cell Function Similar to Impaired Glucose Tolerance (
Diabetes Metab J 2015;39:147-53) - Tae Jung Oh, Se Hee Min, Chang Ho Ahn, Eun Ky Kim, Soo Heon Kwak, Hye Seung Jung, Kyong Soo Park, Young Min Cho
- Diabetes Metab J. 2015;39(3):270-271. Published online June 15, 2015
- DOI: https://doi.org/10.4093/dmj.2015.39.3.270
- 3,189 View
- 34 Download
- 1 Crossref
-
 PDF
PDF PubReader
PubReader -
Citations
Citations to this article as recorded by- Prevalence of Impaired Glucose Tolerance/Prediabetes in Local Adult Obese Population Presenting to A Tertiary Care Hospital
Niktash Khan Hadi, Muhammad Salman Aamir, Tahir Ghaffar, Sulaiman Khan, Siraj ul Islam, Shafiullah Khan, Nizamuddin ., Muhammad Ali
Pakistan Journal of Health Sciences.2023; : 84. CrossRef
- Prevalence of Impaired Glucose Tolerance/Prediabetes in Local Adult Obese Population Presenting to A Tertiary Care Hospital
- Erratum: Figure Correction. A Gut Feeling to Cure Diabetes: Potential Mechanisms of Diabetes Remission after Bariatric Surgery
- Young Min Cho
- Diabetes Metab J. 2015;39(2):175-175. Published online April 20, 2015
- DOI: https://doi.org/10.4093/dmj.2015.39.2.175
- 2,386 View
- 37 Download

 KDA
KDA
 First
First Prev
Prev





